From the research, to the clinic.

Advanced concussion assessment performed using “Vesticam” oculography, and “AxIT” force plate technology.
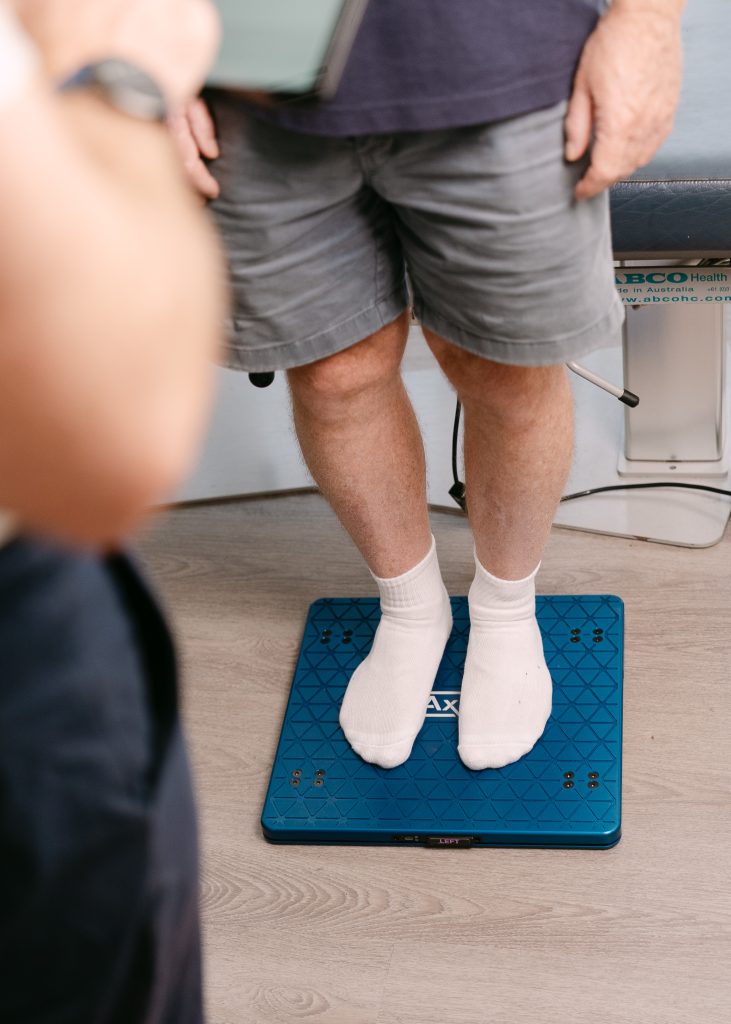
Concussion Management, Baseline Testing and Persistent Post-Concussion Symptoms in Adelaide
Concussion is often misunderstood.
It does not always involve a direct blow to the head. It does not always involve loss of consciousness. And in many cases, standard CT or MRI scans are normal. What matters is the force transmitted to the brain, the symptoms that follow, and how recovery is managed.
At Aevora Health in Malvern, we take an evidence-informed approach to concussion care. That includes clinical assessment, symptom profiling, objective testing where appropriate, guided return-to-activity planning, and support for those whose recovery has not followed the usual timeline.
What is a concussion?
A concussion is a mild traumatic brain injury caused by biomechanical force. In simple terms, the brain is exposed to rapid acceleration, deceleration, or rotational loading that disrupts normal function.
This can happen in contact sport, but also in cycling crashes, falls, gym incidents, car accidents, and any event where force is transmitted to the head and neck region.
Common concussion symptoms
Concussion symptoms vary, but commonly include headache, dizziness, nausea, light or noise sensitivity, blurred vision, fatigue, neck pain, feeling slowed down, trouble concentrating, feeling foggy, irritability, anxiety, or mood change.
One of the most important clinical realities is that concussion is not one single presentation. Different people can present with very different patterns of symptoms, including vestibular issues, visual or oculomotor dysfunction, fatigue, cognitive symptoms, migraine-like features, or mood changes.
That matters because two people can both have a concussion while needing very different management.
What are persistent post-concussion symptoms?
Persistent post-concussion symptoms are ongoing symptoms that continue beyond the expected recovery window after a concussion.
This may include ongoing headaches, dizziness, fatigue, exercise intolerance, visual overload, poor concentration, sleep disruption, irritability, or a lingering sense that you are still not quite right.
Persistent symptoms do not automatically mean something serious has been missed. More often, they mean recovery needs to be assessed more carefully. Ongoing symptoms may be driven by one or more identifiable issues, such as vestibular dysfunction, visual strain, cervical spine involvement, autonomic or exertional intolerance, headache phenotype, sleep disruption, or stress-related load.
This is why generic advice is often not enough.
Why complete rest is no longer the answer
Older concussion advice often centred on complete rest, dark rooms, and waiting.
That is no longer the preferred approach.
The goal is not to do nothing. The goal is to do the right things, at the right time, in the right dose. Early management may involve relative rest, reducing unnecessary aggravation, limiting screen exposure initially, and then progressively reintroducing movement and activity in a controlled way.
In many cases, a carefully graded return to exercise is more helpful than prolonged inactivity.
Why baseline concussion testing matters for sports groups
For clubs, schools and sporting organisations, baseline concussion testing can be a useful part of a broader concussion process.
Baseline data gives you a pre-injury reference point. That can help guide post-injury decision-making, especially when looking at symptoms, balance, visual or vestibular function, exertional response, and return-to-play readiness.
For sporting groups, baseline testing is most valuable when it sits inside a broader system that includes player and parent education, clear removal-from-play rules, timely follow-up after suspected concussion, objective reassessment where needed, and structured return-to-sport decision-making.
Baseline testing is not a magic solution on its own. But it can make post-injury decisions more informed and more defensible.
Ask about team baseline testing
How concussion should be assessed
Concussion assessment should not rely on a single test.
A useful assessment looks at the full picture: symptoms, balance, eye movements, vestibular function, cervical spine involvement, exercise tolerance, and any factors that may be slowing recovery.
At Aevora Health, assessment may include symptom profiling, cervical spine assessment, vestibular and oculomotor testing, balance and postural control assessment, and graded exertional testing where appropriate.
This helps identify what is actually driving symptoms, rather than treating every concussion as though it is the same.
Why return-to-sport decisions matter
Returning too early is not trivial.
Even when symptoms appear to be improving, functional recovery may still be incomplete. For athletes, parents, coaches, and clubs, the key question is not only whether symptoms have settled. It is whether the person is genuinely ready to return.
That is where careful clinical assessment and, where appropriate, objective testing can help guide safer and more confident decisions.
Who this may be for
This service may be relevant if you are an athlete with a recent concussion, a parent concerned about a child’s recovery after sport-related concussion, a club or school wanting preseason baseline concussion testing, or someone still dealing with headaches, dizziness, fatigue, or brain fog weeks after a concussion.
It may also be relevant if you are dealing with persistent post-concussion symptoms and want a more structured assessment.
Concussion care in Adelaide
If you are looking for concussion management in Adelaide, sports concussion baseline testing, or help with persistent post-concussion symptoms, the next step should be careful assessment rather than guesswork.
At Aevora Health, Malvern, we provide evidence-informed concussion assessment and management for athletes, active adults, and sporting groups seeking a more measured, practical, and objective approach.
References
- Patricios JS, Schneider KJ, Dvorak J, et al. Consensus statement on concussion in sport: the 6th International Conference on Concussion in Sport—Amsterdam, October 2022. British Journal of Sports Medicine. 2023;57(11):695-711. doi:10.1136/bjsports-2023-106898.
- Echemendia RJ, Burma JS, Bruce JM, et al. Acute evaluation of sport-related concussion and implications for the Sport Concussion Assessment Tool (SCAT6) for adults, adolescents and children: a systematic review. British Journal of Sports Medicine. 2023;57(11):722-735. doi:10.1136/bjsports-2022-106661.
- Echemendia RJ, Brett BL, Broglio S, et al. Sport Concussion Assessment Tool 6 (SCAT6). British Journal of Sports Medicine. 2023;57(11):622-631. doi:10.1136/bjsports-2023-107036.
- Patricios J, Schneider GM, van Ierssel J, et al. Sport Concussion Office Assessment Tool – 6 (SCOAT6). British Journal of Sports Medicine. 2023;57(11):651-667. doi:10.1136/bjsports-2023-106859.
- Leddy JJ, Haider MN, Ellis MJ, et al. Early Subthreshold Aerobic Exercise for Sport-Related Concussion: A Randomized Clinical Trial. JAMA Pediatrics. 2019;173(4):319-325.
- Rytter HM, Graff HJ, Henriksen HK, et al. Nonpharmacological Treatment of Persistent Postconcussion Symptoms in Adults: A Systematic Review and Meta-analysis and Guideline Recommendation. JAMA Network Open. 2021;4(11):e2132221. doi:10.1001/jamanetworkopen.2021.32221.
- Feddermann-Demont N, Echemendia RJ, Schneider KJ, et al. What domains of clinical function should be assessed after sport-related concussion? A systematic review. British Journal of Sports Medicine. 2017;51(11):903-918. doi:10.1136/bjsports-2016-097403.
- Davis GA, Echemendia RJ, Ahmed OH, et al. Child SCAT6. British Journal of Sports Medicine. 2023;57(11):636-647. doi:10.1136/bjsports-2023-106982.

What Is AxIT — And Why Consider Screening at Aevora Health?
Most people are used to health care being built around symptoms.
You are sore. You feel weak. One side feels different. Your knee is “better”, but you still do not trust it.
Your rehab looks fine on paper, yet you are not back to running, jumping, lifting, or changing direction with confidence.
That is where objective testing becomes useful.
At Aevora Health, AxIT helps us look beyond guesswork and measure physical qualities that actually matter: strength, force output, asymmetry, balance, power, and how those change over time.
What is AxIT?
AxIT is an assessment system used to measure physical performance in a more objective way.
Depending on the tests selected, it can be used to assess:
- isolated muscle strength
- side-to-side differences
- force production
- rate of force development
- jump performance
- balance and movement control
In plain terms, it helps answer a more useful question than “does this feel okay?”
It helps answer: what is actually going on here, and what should we do about it?
Why that matters
A lot of people are told they need to get stronger, more stable, or more explosive.
That may be true. But compared with what?
Without a baseline, it is easy to rely on impression alone. Objective screening gives us something better:
- a clearer starting point
- a way to spot meaningful deficits
- a way to compare one side with the other
- a way to track whether rehab or training is actually working
That is particularly useful when symptoms are only part of the story.
Pain can improve before capacity has fully returned. Confidence can lag behind symptom change. And sometimes the opposite happens — people still feel flat or cautious even though the key physical markers are improving.
Testing helps bring clarity to that.
What might be tested?
That depends on the person and the question we are trying to answer.
At Aevora Health, screening is selected around your presentation, not done as a generic battery for the sake of it.
Your assessment may include tests relating to:
- hip, knee, calf, shoulder, or trunk strength
- squat performance and load tolerance
- countermovement jump performance
- isometric mid-thigh pull force
- asymmetry between limbs
- force production in positions relevant to your injury or sport
For one person, that may help explain why their knee still does not tolerate stairs, running, or single-leg loading. For another, it may show whether they are actually ready to return to sport. For someone else, it may simply provide a useful baseline before problems develop.
Who tends to benefit most?
People recovering from injury
If you are coming back from knee pain, tendon pain, ankle issues, surgery, hip pain, hamstring problems, or recurrent flare-ups, screening can help identify what is still lagging behind.
Runners and sporting athletes
If your activity involves absorbing force, producing force, or tolerating repeated loading, objective testing can highlight deficits that are easy to miss in day-to-day training.
People stuck in the “better, but not right” phase
This is one of the most useful groups to test. Symptoms may have improved, but capacity has not fully come back. That gap matters.
People who want to be proactive
Not everyone needs to wait for a breakdown. Screening can be useful for people who want a clearer picture of their current physical capacity and want to pick up weaknesses or asymmetries early.
People who like clear data
Some people engage much better when progress is visible. Rather than being told they are improving, they can actually see what has changed.
Why this can improve care
The real value of AxIT is not in the device itself. It is in the decisions that follow.
Better data can help us:
- choose more targeted rehab
- progress loading with more confidence
- identify whether one side is still underperforming
- improve buy-in to a management plan
- decide when to push, when to hold, and what to re-test
That is especially relevant in a clinic model like Aevora Health, where the goal is not just short-term symptom relief, but better long-term physical resilience.
Why re-testing matters
A single assessment is useful.
Re-testing is where it becomes much more valuable.
Once a baseline is established, we can come back later and ask:
- Has strength improved?
- Has the asymmetry narrowed?
- Is force production moving in the right direction?
- Has capacity returned, or have symptoms simply settled?
That gives both practitioner and patient a much clearer picture of progress.
Is this only for athletes?
No.
Athletes often like objective testing because return-to-play decisions matter. But the same principles are useful for everyday people.
You do not need to be elite to benefit from understanding your physical capacity more clearly.
For many people, the value is simpler than that: less guesswork, better direction, and a more personalised plan.
AxIT at Aevora Health
At Aevora Health, AxIT is used when objective measurement is likely to improve decision-making.
That may be in the context of rehab, performance, prevention, or simply trying to understand why the same issue keeps recurring.
It is not there to make an assessment look more impressive.
It is there to help answer practical questions, guide a smarter plan, and show whether meaningful change is actually happening.
Thinking about booking?
If you want a clearer understanding of your current physical capacity — whether for injury recovery, performance, or prevention — AxIT screening may be a useful place to start.
Book online to arrange an assessment at Aevora Health.
References
- Lichtenstein E, Wagner J, Knaier R, et al. Norm Values of Muscular Strength Across the Life Span in a Healthy Swiss Population: The COmPLETE Study. Sports Health. 2023;15(4):547-557. doi:10.1177/19417381221116345.
- Douma RKW, Soer R, Krijnen WP, Reneman MF, van der Schans CP. Reference values for isometric muscle force among workers for the Netherlands: a comparison of reference values. BMC Sports Science, Medicine and Rehabilitation. 2014;6:10.
- Buckinx F, Croisier JL, Reginster JY, et al. Reliability of muscle strength measures obtained with a hand-held dynamometer in an elderly population. Clinical Physiology and Functional Imaging. 2017;37(3):332-340.
- Whiteley R, Jacobsen P, Prior S, Skazalski C, Otten R, Johnson A. Correlation of isokinetic and novel hand-held dynamometry measures of knee flexion and extension strength testing. Journal of Science and Medicine in Sport. 2012;15:444-450.
- Florencio LL, Martins J, da Silva MRB, et al. Knee and hip strength measurements obtained by a hand-held dynamometer stabilized by a belt and an examiner demonstrate parallel reliability but not agreement. Physical Therapy in Sport. 2019;38:115-122.
- Maffiuletti NA, Aagaard P, Blazevich AJ, Folland J, Tillin N, Duchateau J. Rate of force development: physiological and methodological considerations. European Journal of Applied Physiology. 2016;116:1091-1116.
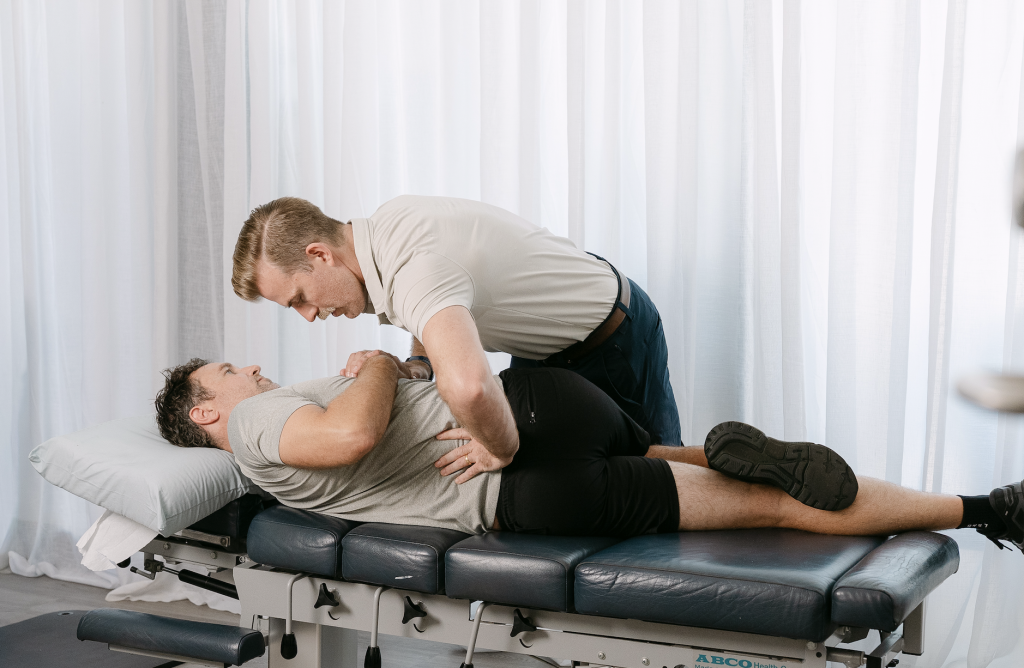
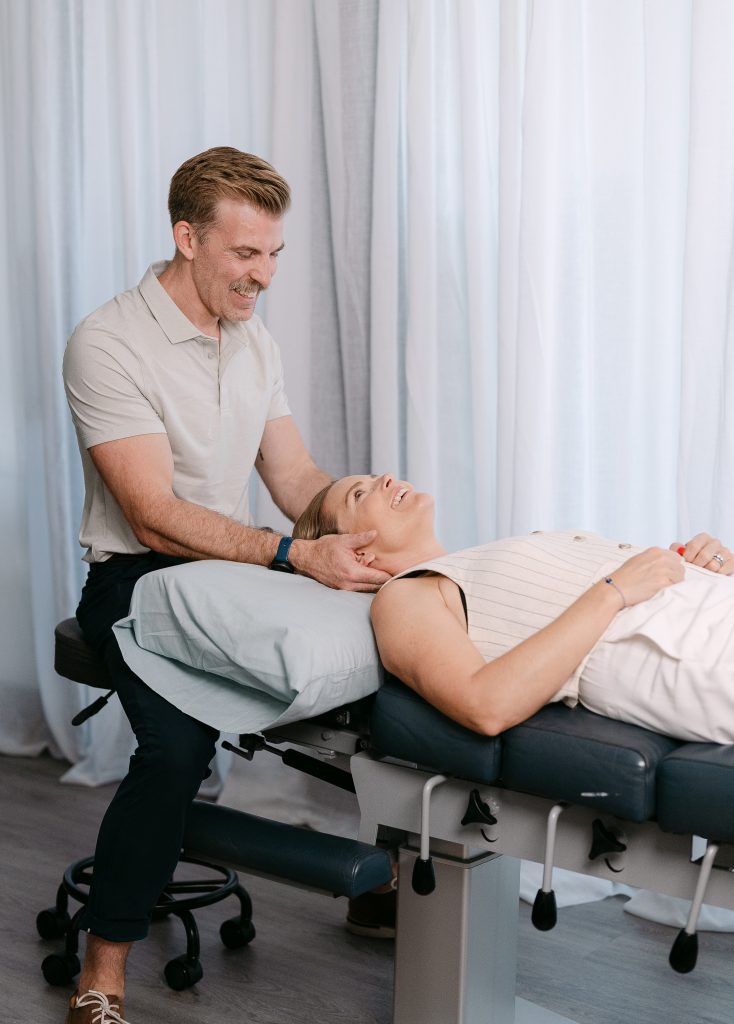
How spinal adjustments and manual therapy may help: more than a mechanical effect
When most people think of a spinal adjustment, they think of clicking, cracking, and bones being “put back in.” That is not a particularly good explanation.
A better explanation is this: spinal adjustments and other forms of manual therapy are ways of delivering a specific mechanical input to the nervous system.
That matters because pain, stiffness, muscle tension, and movement quality are not determined by tissues alone. They are also shaped by how the brain and nervous system interpret sensory input from joints, muscles, and surrounding soft tissues. In many cases, especially ongoing spinal pain, the therapeutic effect of manual therapy appears to be less about changing structure and more about changing the way the system is processing threat, tension, and movement.
What is an adjustment, really?
A spinal adjustment is typically a high-velocity, low-amplitude input to a joint. It is small. It is fast. And despite the familiar “crack,” the sound itself is not the treatment. That pop is simply gas moving within the joint. It does not mean something has been put back into place, and it is not required for benefit.
What seems to matter more is the rapid stretch applied to tissues around the joint, particularly muscles and joint receptors. That fast, novel input stimulates mechanoreceptors and muscle spindles, sending a large burst of sensory information into the nervous system.
The nervous system explanation
The most useful modern explanation for manual therapy is neurophysiological.
First, manual therapy may help dampen pain. Mechanical input from joints and muscles can alter nociceptive processing at the spinal cord and brainstem level. In plain English: a well-timed sensory input can temporarily reduce how strongly pain is being turned up. This aligns with the broader idea that movement-related sensory signals can compete with, and modulate, pain signalling.
Second, manual therapy may influence muscle tone. Anyone who has felt “locked,” guarded, or stiff knows that pain is often accompanied by protective muscle activity. A rapid stretch can briefly alter the gain of the muscle spindle system and change how muscles are being controlled. Clinically, this can feel like less tightness, easier movement, or less resistance through range.
Third, it may improve proprioception and body awareness. Joints and muscles are constantly reporting to the brain about position, motion, and load. When that sensory reporting is poor, movement can become less efficient, less coordinated, and in some people, more provocative. A spinal adjustment or mobilisation may provide an amplified sensory signal that helps the brain update its internal map of that area. The result is not just less pain, but often smoother, more confident movement.
This is one reason manual therapy can be useful even when the aim is not simply pain relief. Sometimes the benefit is creating a short-term window in which movement becomes easier, exercise becomes more tolerable, and the patient regains trust in the region.
What does the research suggest?
The literature does not support simplistic claims that manual therapy “fixes” everything mechanically. But it does support several clinically useful effects.
Research has shown that spinal manipulation can alter pain sensitivity, with systematic review data suggesting measurable hypoalgesic effects in at least some patients. Experimental work has also found reductions in hyperalgesia after manipulation, and mechanistic studies have pointed toward involvement of non-opioid descending inhibitory pathways.
Other research has shown that manipulative inputs can provoke muscle spindle discharge in a way that differs from ordinary movement or slow passive motion. That supports the idea that manual therapy delivers a distinct sensory stimulus, not merely a generic stretch.
There is also emerging work suggesting that manual therapy may influence higher-order pain processing. In chronic low back pain, spinal manipulative therapy has been associated with changes in anticipated pain, fear of movement, and brain activity in regions involved in salience and affective processing. That is important, because persistent pain is not just a tissue issue. It is often a whole-system issue involving sensation, prediction, protection, and behaviour.
So what are the real benefits?
For the right person, at the right time, manual therapy may help by:
- reducing pain in the short term
- easing protective muscle guarding
- improving movement quality and range
- enhancing proprioception and body awareness
- reducing fear around movement
- creating a better platform for exercise rehabilitation
That last point is key.
Manual therapy is usually best viewed as an adjunct, not the whole treatment. It can open the door, but exercise, loading, education, sleep, general activity, and confidence-building are what usually keep it open.
Where manual therapy fits in good care
A sensible modern model is not “adjust forever because your spine keeps going out.”
It is: use manual therapy when it is likely to help modulate pain, reduce guarding, or improve movement; then use that window to build capacity.
That may involve mobility work, strength training, graded exposure to feared movements, postural variety, walking, breathing drills, or return-to-sport progressions. The exact mix depends on the person in front of you.
So yes, spinal adjustments can be helpful. But the strongest case for them is not mystical, and it is not purely mechanical. It is that they provide a targeted sensory input to a nervous system that may be overprotective, poorly coordinated, or sensitised.
That is a much more plausible explanation. And it fits both modern pain science and what many patients actually experience in practice.
References
- Coronado RA, Gay CW, Bialosky JE, Carnaby GD, Bishop MD, George SZ. Changes in pain sensitivity following spinal manipulation: a systematic review and meta-analysis. Journal of Electromyography and Kinesiology. 2012;22(5):752-767.
- Ellingsen D-M, Napadow V, Protsenko E, Mawla I, Kowalski MH, Swensen D, et al. Brain mechanisms of anticipated painful movements and their modulation by manual therapy in chronic low back pain. The Journal of Pain. 2018;19(11):1352-1365.
- Melzack R, Wall PD. Pain mechanisms: a new theory. Science. 1965;150(3699):971-979.
- Mohammadian P, Gonsalves A, Tsai C, Hummel T, Carpenter T. Areas of capsaicin-induced secondary hyperalgesia and allodynia are reduced by a single chiropractic adjustment: a preliminary study. Journal of Manipulative and Physiological Therapeutics. 2004;27(6):381-387.
- Pickar JG. Neurophysiological effects of spinal manipulation. The Spine Journal. 2002;2(5):357-371.
- Pickar JG, Sung PS, Kang Y-M, Ge W. Response of lumbar paraspinal muscle spindles is greater to spinal manipulative loading compared with slower loading under length control. The Spine Journal. 2007;7(5):583-595.
- Schmid A, Brunner F, Wright A, Bachmann LM. Paradigm shift in manual therapy? Evidence for a central nervous system component in the response to passive cervical joint mobilisation. Manual Therapy. 2008;13(5):387-396.
- Skyba DA, Radhakrishnan R, Rohlwing JJ, Wright A, Sluka KA. Joint manipulation reduces hyperalgesia by activation of monoamine receptors but not opioid or GABA receptors in the spinal cord. Pain. 2003;106(1-2):159-168.
- Sung PS, Kang Y-M, Pickar JG. Effect of spinal manipulation duration on low threshold mechanoreceptors in lumbar paraspinal muscles: a preliminary report. Spine. 2005;30(1):115-122.
